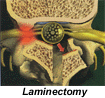
Lumbar Laminectomy
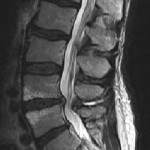 Summary:
Summary:- Stenosis compresses the spinal nerves causing pain
- Laminectomy uses minimally invasive techniques to decompression nerves to give more room
- Typically discharged the day after surgery
Introduction
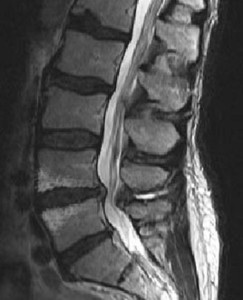 What is Spinal Stenosis?
What is Spinal Stenosis?
Spinal Stenosis occurs over time as we age and slowly compresses the spinal cord, which results in low back pain and often numbness, weakness and pain in the legs. Symptoms are often made worse with walking. In severe cases, the bladder and bowel may also be affected. Though there are many potential causes for spinal stenosis, the most common cause is the natural wear and tear brought upon by aging. As we get older, the ligaments of the spine that hold the bones together can thicken and pinch the nerves that run through and out of the spinal canal. In other instances, the nerve pinching may be caused by bone spurs as they grow throughout the bones of the lumbar spine. Additionally, collapse of the disc spaces between the vertebrae, called spondylosis, can occur which increases pressure on the joints between the vertebrae. These joints, called facet joints, begin to enlarge and sometimes become unstable requiring additional fusion surgery in some cases (see Lumbar Fusion without Metal Screws and Rods).
Alternatives to Surgery
Generally, conservative treatment, or non-surgical treatment, is helpful in the early phase of stenosis. At times, conservative therapy such as bed rest, medication, injections, physical therapy, or traction may relieve the symptoms associated with a herniated disc, bone spurs or spinal stenosis and avoid the need for surgery. However, when conservative therapies have proven ineffective, a Lumbar Laminectomy may be considered.
Diagnostic tests are required prior to surgery, which typically consists of Magnetic Resonance Imaging (MRI) or a Computed Tomography (CT) scan. A MRI can indicate the degree of bone spurring or disc space collapse and allow your neurosurgeon to perform the procedure according to your level of severity. Additional pre-operative tests such as a myelogram may be required to determine the degree of stenosis and to diagnose the problem most accurately and prepare you for surgery.
What is the Procedure?
The surgery used to treat spinal stenosis is the lumbar laminectomy. It is somewhat more invasive than a Microdiscectomy, but typically well tolerated. Depending on the levels of the spine requiring decompression(i.e. how “long” the compressed segment of the spine is), an incision is made in the lumbar area, and the lamina, or outer bone of the vertebra, is exposed. With the use of specialized instruments and an operating microscope, the outer bone is removed along with any other sources of compression. The spinal nerve and the nerve roots that connect to the legs are explored and decompressed. The lumbar laminectomy can last one to two hours depending on the number of levels involved.
What is the Recovery Time?
After surgery, the leg symptoms are typically improved to the extend that you are walking the night of surgery and generally can return home the next day. Following the surgery, minor discomfort resulting from the incision is common, but temporary. If such pain occurs, it can be relieved through the use of mild pain medication. Additionally, persistent numbness, weakness, and pain along the path of the now decompressed nerve may still occur, but such symptoms are generally temporary and improve over time.
What are Surgical Risks?
A Lumbar Laminectomy procedure is done using minimally invasive techniques, and with the help of a surgical microscope, which allows for reduced tissue trauma and hence faster healing times. In most cases, the patient is released from the hospital the next day and is able to return to many of the daily activities performed prior to the surgery. There are generally no additional restrictions after 1 to 3 months post-surgery. Despite an overall success rate of 80 to 90%, there are, as with all procedures, certain risks to be made aware of. These risks include, but are not limited to: infection, excess bleeding, no relief of symptoms, excess scarring, increased neurological dysfunction, bladder or bowel problems and anesthetic complications.
Tri-State Neurosurgical Associates-UPMC
Administrative Oakland Office Address:
Presbyterian University Hospital
Department of Neurosurgery
Suite 5C
200 Lothrop Street
Pittsburgh, PA 15213
Phone: 1-888-234-4357
© 2013 Tri-State Neurosurgical Associates – UPMC



 Dr. Maroon received an athletic scholarship to Indiana University in Bloomington, Indiana where as an undergraduate, he was named a Scholastic All-American in football. Dr. Maroon has successfully maintained his personal athletic interests through participation in 9 marathons and more than 72 Olympic-distance triathlon events. However, his greatest athletic accomplishment is his participation in 8 Ironman triathlons (Hawaii – 1993, 2003, 2008, 2010, 2013; Canada – 1995; New Zealand – 1997; Germany – 2000), where he usually finishes in the top 10 of his age group. Recently, in July 2012 and 2013, he finished second and third, respectively, in his age group in the Muncie, Indiana half Ironman triathlon. In October 2013 he completed his 5th World Championship Ironman in Kona, Hawaii.
Dr. Maroon received an athletic scholarship to Indiana University in Bloomington, Indiana where as an undergraduate, he was named a Scholastic All-American in football. Dr. Maroon has successfully maintained his personal athletic interests through participation in 9 marathons and more than 72 Olympic-distance triathlon events. However, his greatest athletic accomplishment is his participation in 8 Ironman triathlons (Hawaii – 1993, 2003, 2008, 2010, 2013; Canada – 1995; New Zealand – 1997; Germany – 2000), where he usually finishes in the top 10 of his age group. Recently, in July 2012 and 2013, he finished second and third, respectively, in his age group in the Muncie, Indiana half Ironman triathlon. In October 2013 he completed his 5th World Championship Ironman in Kona, Hawaii.